Copyright © 2007-2018 Russ Dewey
Desensitization and Exposure Therapies
Desensitization was the first therapy to be called a behavior therapy. It was self-consciously designed using insights from laboratory work on conditioning, and it focused directly on problem behavior rather than trying to treat an underlying mental illness.
Desensitization was proposed by the South African psychiatrist Joseph Wolpe (pronounced VOLE-py). Desensitization was the first widely-adopted therapy based on a behavioral principles, so Wolpe became known as the father of behavior therapy.
Wolpe's inspiration came from experiments by Masserman (1943) who made cats "neurotic" by giving them electric shocks in a box. Soon the cats acted anxious when put in the box.
Masserman observed that the cats lost their "neurosis" if they were fed in the box. He interpreted this in psychodynamic terms, as "breaking through the motivational conflict."
Wolpe saw the same events as conditioning. Shocking the cats in the box created an association between that location (or the act of being put in the box) and a painful aftereffect. A CER was established, as the sight of the box provoked anxiety.
By feeding the cat in the box, Masserman counteracted the conditional emotional response (CER). Now the sight of the box predicted food instead of a shock, so the anxiety disappeared.
Wolpe called this counterconditioning. That phenomenon was discovered by one of Pavlov's students in 1912 (Wolpe and Plaud, 1997).
In counterconditioning, a conditional response is eliminated by replacing it with another, incompatible response. At first, before discovering the work of Pavlov's student, Wolpe called the pattern reciprocal inhibition. Wolpe felt the responses of anxiety and eating inhibited or prevented each other.
Whatever it is called, the procedure works. Wolpe replicated Masserman's work, showing that cats would lose their fear of a box where they had been shocked, if he fed them first at a distance, then closer to the box where previously they were shocked. Eventually the cats lost their fear of the box entirely.
How did Masserman produce neurotic cats? How did he then reduce the fear?
Wolpe devised a procedure for using reciprocal inhibition (or counterconditioning) in humans. First, he taught the patient to relax deeply, using Jacobsonian progressive relaxation.
In Jacobsonian progressive relaxation, a client is taught to relax muscle groups, starting with toes, working up to shoulder and neck and forehead muscles. First a muscle group is tensed, then completely relaxed, while the client tunes in on that distinction, learning how to recognize total muscle relaxation.
That takes a few sessions to master, but patients gradually learn to relax completely, at will. Then Wolpe encouraged patients to visualize or imagine the anxiety-arousing stimulus while remaining relaxed.
Wolpe had patients make what he called a fear hierarchy (actually an ordered list) from least-fearsome to most-fearsome images relating to their phobia. For example, if the patient was snake-phobic, he or she might produce this list:
1. A tiny snake 50 feet away (the least fearsome image)
2. A larger snake 30 feet away
3. A large snake 10 feet away
4. A large snake on the ground right in front of me
5. A snake bumping against my foot then slithering away
6. A snake being placed in my hands
7. A snake wrapping itself around my arm
8. A snake slithering up my arm toward my neck
9. A snake taking a big bite out of my cheek
10. Falling into a pit of poisonous snakes (the most fearsome image)
The patient started, fully relaxed, by imagining the least anxiety-arousing image (#1). If the patient felt any anxiety while doing this, he or she would raise a finger, and Wolpe would immediately return to hypnosis-like relaxation instructions.
How was desensitization therapy conducted, in Wolpe's original procedure?
The patient moved on to the next image only when able to stay fully relaxed while imagining the previous image. Given enough time, a snake-phobic individual could work through the entire list while remaining relaxed.
When the client could imagine the worst, most fearsome scene while fully relaxed, the conditional emotional response (CER) of anxiety was undone or extinguished. To use Pavlov's terminology, the conditional stimulus (thought of a snake) no longer elicited a conditional response of anxiety.
As usually occurs with extinction procedures, there might be some spontaneous recovery of the extinguished response. By the next therapy session, some fear might be back. If so, Wolpe repeated the procedure until the patient could again stay fully relaxed while imagining the most fearsome stimulus.
Desensitization works, and it is simple to administer. However, the procedure Wolpe developed could take months to unfold. First the patient had to learn Jacobsonian progressive relaxation, then it was time to work through the lengthy fear hierarchy, with treatment halted each time a patient raised a finger.
As noted in Chapter 8 (Animal Behavior and Cognition) certain types of phobias seem to be "prepared" by evolution. Those are more difficult to treat.
Biologically prepared phobias include snake, spider, and small animal phobias. Even these instinctive fears usually yield to desensitization in the long run. Less biologically-based phobias such as test anxiety and fear of flying often can be eliminated quickly.
Years after Wolpe developed desensitization, historians of psychology and Wolpe himself pointed out his procedure was anticipated almost completely in a 1924 study by Mary Cover Jones, then at Teachers College of Columbia University. She was doing research under the guidance of John Watson.
Watson had shown, in a 1921 experiment with a child called Little Albert, that fear could be induced through Pavlovian conditioning. Little Albert was 11 months old when Watson brought him into the laboratory.
Watson found that striking a steel bar, producing a sharp sound, made Little Albert cry. Next, Watson introduced a pet rat, and Albert showed no fear. When Albert reached out to touch the rat, Watson struck the steel bar.
After repeating this association seven times, Albert "not only became greatly disturbed at the sight of a rat, but this fear had spread to include a white rabbit, cotton wool, a fur coat, and the experimenter's hair. It did not transfer to his wooden blocks and other objects very dissimilar to the rat." (Jones, 1924)
In other words, Watson had established a conditional emotional response (CER) as described in Chapter 5. Little Albert also showed generalization by reacting to furry stimuli that somewhat resembled the rat.
At that point, Little Albert was removed from the hospital, so Watson could do no further research. Three years later, in a study published in 1924, Mary Cover Jones decided to see if such a fear could be extinguished.
Jones located a little boy named Peter, aged 2 years and 10 months. "He was afraid of a white rat, and this fear extended to a rabbit, a fur coat, a feather, cotton wool, etc., but not to wooden blocks and similar toys." As Mary Cover Jones commented, he "seemed almost to be Albert grown a bit older."
Jones decided to eliminate Albert's fear of the rabbit by bringing the rabbit into the play room and gradually moving the rabbit closer to Albert. She reported the following stages of progressively closer contact:
A. Rabbit anywhere in the room in a cage causes fear reactions.
B. Rabbit 12 feet away in cage tolerated.
C. Rabbit 4 feet away in cage tolerated.
D. Rabbit 3 feet away in cage tolerated.
E. Rabbit close
F. Rabbit free in room tolerated.
G. Rabbit touched when experimenter holds it.
H. Rabbit touched when free in room.
I. Rabbit defied by spitting at it, throwing things at it, imitating it.
J. Rabbit allowed on tray of high chair.
K. Squats in defenseless position beside rabbit.
L. Helps experimenter to carry rabbit to its cage.
M. Holds rabbit on lap.
N. Stays alone in room with rabbit.
O. Allows rabbit in play pen with him.
P. Fondles rabbit affectionately.
Q. Lets rabbit nibble his fingers.
Like Wolpe's "fear hierarchy," this resulted in a gradual exposure to more and more of the feared stimulus. As a result "Peter progressed from a great fear of the rabbit to a tranquil indifference and even a voluntary pat on the rabbit's back when others were setting the example."
Jones's procedure resembled desensitization in another way. Peter suffered a setback: spontaneous recovery of his fear. This occurred after he got scarlet fever and had to go to a hospital for two months. When he was returning from the hospital, a large dog, running past, jumped on Peter and his nurse as they were entering a taxi, frightening them both.
Jones noted a "precipitate descent back to the original fear level" when Peter returned to the clinic. Jones speculated that the incident with the dog aggravated Peter's fears and set him on edge. That is certainly possible, or Peter's fear of the rabbit might have returned anyway due to spontaneous recovery.
Jones eliminated the fear again, this time using food as a counter-conditioning stimulus. She called it "unconditioning." As Peter sat in a high chair and ate from a tray, the rabbit was set down 12 feet away.
Peter began to cry, but another child (Lawrence) said, "Oh, rabbit" and then "clambered down, ran over and looked in the cage at him." Peter followed closely and watched.
By the 21st session, Peter was eating candy in the high chair with the rabbit directly in front of him, on the tray. When both the rabbit and Peter were allowed free movement in the room, Peter cried out "I don't want him" and withdrew, but when another child patted the rabbit, then "Peter wanted the rabbit on his lap, and held it for an instant."
Finally, Mary Cover Jones wrote, "In one of our last sessions, Peter showed no fear although another child was present who showed marked disturbance at the sight of the rabbit." Peter's fear had been extinguished again.

Mary Cover Jones
In short, Jones pioneered many elements of desensitization therapy. Her procedure resembled a variation called in vivo desensitization (discussed on the next page). It actually works better than Wolpe's technique, according to research carried out in the 1970s and 1980s.
Wolpe started calling Jones "the mother of behavior therapy" in the 1970s. Jones, who lived from 1896 to 1987, was still alive to appreciate the credit.
Exposure Therapies
Desensitization was such a successful therapy that it became very important to behavior therapists. It established the credibility of their approach, delivering on the promise of therapy based on experimental evidence.
Researchers were unsure at first about which elements of Wolpe's procedure were necessary. Was the relaxation training really necessary? Apparently not; clients did just as well if they did not learn to relax before the therapy.
Was the fear hierarchy used by Wolpe necessary? Controlled comparisons showed that it was not.
People lost their fears even more quickly if exposed to later items on the list first, without working through the easier items. The crucial variable was exposure to the feared situation, for a sustained period of time, in a safe setting, so the fear reaction could burn out.
What is exposure therapy?
As these findings came out, a quick, extreme version of desensitization was tested in the 1970s. It was called flooding or immersion therapy. Eventually it was simply called exposure therapy.
In exposure therapy, a client is exposed to a safe version of the fearsome stimulus at maximum intensity. The anxiety reaction burns out and is extinguished.
In comparison after comparison, exposure therapy worked as well or better than progressive desensitization (the Wolpe approach) and it took much less time. Clients no longer had to learn progressive relaxation or work through a lengthy fear hierarchy.
Hans Eysenck found that time of exposure was critically important in this type of therapy. That accorded with data from conditioning laboratories, where length of exposure was the variable most directly correlated with extinction.
Patients with a great fear of spiders, who were exposed to spiders for two minutes in a laboratory setting, did not overcome their fear of spiders. In fact, their fear became worse because the exposure time was not long enough. If the exposure was longer, however, extinction occurred. (Cunningham, 1984)
Exposure therapy was the only therapy that worked for obsessive hand-washing, in Eysenck's experience. Some people washed their hands hundreds of times a day, until their hands were red and sore.
A deeply rooted anxiety about contamination seemed to be involved. Eysenck tried an extinction procedure. He had compulsive hand-washers immerse their hands in a barrel of rubbish, then just sit there with contaminated hands for several hours, without being allowed to wash them.
How did Eysenck claim to cure 90% of compulsive hand-washers?
"Immediately there is a welling-up of anxiety and fear," said Eysenck. "The patient is forced to remain there for an hour or two. Eventually the emotion is gone....
Even doing it once produced such a change in the attitude and emotions of the subject." The treatment worked for 90 percent of the patients, he added. (Cunningham, 1984)
What is in vivo desensitization?
Exposing a spider-phobic person to spiders, or a compulsive hand-washer to dirty hands, is an example of in vivo (in VEE-vo) desensitization. In vivo is a Latin phrase meaning in life. The client is exposed to the real thing, the actual feared stimulus, rather than imagining fearful scenes.
In retrospect, Mary Clover Jones used an in vivo procedure with Peter, the almost-three-year-old who feared rabbits. He lost his fear when introduced gradually to a real rabbit. By the end of the experiment, he could pat the bunny without fear.
Professionals find that this type of therapy must be approached carefully when clients have strong phobias. Some clients have panic reactions during flooding procedures, particularly when prepared phobias like snake and spiker phobias are involved.
However, panic reactions are not always discouraged in exposure therapy. If the panic reaction occurs in a safe situation (in the company of the therapist) it will simply burn itself out in 10 or 20 minutes.
This results in a re-education of the neurons involved in the CER (conditional emotional response). If a feared stimulus remains present, but the panic reaction subsides, maybe there is nothing to fear.
This learning occurs on a deep level, just like the original fear. (Recall that classical conditioning is the oldest, most primitive form of learning, not requiring conscious deliberation.)
The extinction procedure demonstrates a lack of contingency, a lack of prediction, between the feared stimulus and the anxiety reaction. The neurons activating the alarm system of the amygdala are re-educated, taught through experience that a previously-feared stimulus actually does not predict danger. This works when verbal therapies fail.
In cases of non-biological phobias such as elevator phobias, clients may be asked to drink a water and caffeine mixture to induce a panic reaction. The client rides up and down in an elevator, has a panic attack, lets the reaction run its course in 20-30 minutes, and extinction occurs.
How is drug-induced relaxation used to treat fear of flying?
In vivo desensitization is much faster than Wolpe's original procedure. Dramatic improvements can be achieved in a few treatment sessions, instead of many months.
In vivo desensitization is easily combined with drug-facilitated relaxation. Meldmand and Hatch (1969) treated an airplane phobia by administering an anxiety-reducing drug (methoxyflorone) to clients who were taken aloft in a plane.
This eliminated their fear of flying, and the clients were able to resume using commercial airlines. In vivo desensitization remains the treatment of choice for airplane phobias, aided if necessary by anxiety-reducing tranquilizers.
Extinction of CERs in Therapy
Desensitization started as a lengthy (multi-month) therapy involving deep relaxation and imagination. It evolved into brief, exposure-based extinction therapies, partly based on the insight of Hans Eysenck and others that length of exposure was the key variable aiding extinction of a response.
Eysenck offered the opinion that "All neuroses are essentially conditioned emotional responses" (Cunningham, 1984). Eysenck's logic was as follows: mental disturbances commonly involve troublesome emotional reactions to specific situations (just as Ellis said in connection with his therapy).
People seek therapy because they are unable to control these reactions on their own. That is not surprising: Pavlovian conditioning is a primitive process involving deep regions of the brain.
Conditional Emotional Responses (CERs) evolved on earth long before language evolved. Perhaps it is not surprising that people cannot talk themselves out of their fears, and they cannot stop feeling anxious just by trying.
The result? People seek help. They go to a therapist because they cannot stop having the unpleasant emotions. A talking therapy, no matter what type it is, generally involves discussing the problems that cause anxiety. That is exposure to the anxiety-causing stimulus, and ultimately it causes extinction.
Consider how Carl Rogers approached counseling. He had no system for "analyzing" people or giving advice. All he did was listen, try to understand, and provide people with a comfortable, safe environment to explore their issues.
That is the ideal setting for extinction of anxiety responses. Previously forbidden thoughts and feelings are aired out, discussed with the therapist, perhaps weekly, perhaps for months. Eventually the troubling issues lose their sting.
How can non-behavioral therapies be interpreted as extinction procedures?
Talking about the same old problems every week might actually become boring. A client may decide to move on to other issues, if there are any. If not, the client may decide to stop the therapy, because it succeeded.
In this sense, Eysenck may have been correct that all "neuroses" are conditional emotional responses, and all treatment is Pavlovian extinction. Eysenck's statement is an oversimplification, because therapy can have a problem-solving function, or an exploring function, neither of which has much to do with extinguishing CERs.
On the other hand, the reason problem-solving and exploring are necessary in the first place might be a person's reactions to emotional hurts or complexes (in Jung's use of the term). Then Eysenck might have a point. A person must get over having strong negative emotions in order to think rationally about important issues.
Eysenck became famous for an article he published in 1952 titled, "The Effects of Psychotherapy: An Evaluation." In that article he argued that psychotherapy outcome research required comparison to a baseline rate of spontaneous recovery, to see if therapies made any difference.
Eysenck suggested that such a baseline rate could be gleaned from data about the percentage of patients released from mental hospitals. He wrote:
The percentage of neurotic patients discharged annually as recovered or improved from New York state hospitals is 70 (for the years 1925-
The consolidated amelioration rate of New York state hospitals, 1917-
Eysenck then produced summary data for therapy outcome research. The average number of cases rated "improved" or "very improved" after psychotherapy was 64% across all studies. This was essentially the same as the baseline rate of "spontaneous remission" defined as discharges from mental hospitals.
One could quarrel with Eysenck's assumption that admission to a mental hospital is equivalent to "no treatment" or "no therapy." For most people, admission to a mental hospital would create a strong incentive to get better, in order to leave the hospital.
Therefore, what Eyesenck really documented was a strong form of contingency management. The contingency is, "Get better or you lose your freedom." That appears to work about 60-70% of the time.
What 1952 publication by Eysenck became famous?
Eysenck's claim, in 1952, that psychotherapy produced no better outcome rates than spontaneous remission, was a challenge to researchers. It began decades of therapy-outcome research.
Over time, a pattern emerged. All therapies, regardless of the theoretical system, had about the same success rate. About two-thirds of clients improved.
Even people who received no formal psychotherapy tended to improve about two-thirds of the time, over a period of years. Perhaps all different forms of therapy, formal and informal, are at root exposure therapies, with similar percentages of happy outcomes.
In other words, anybody who talks over their problems with a therapist or a friend is airing thoughts and emotions in a safe environment. Extinction of anxiety or fear responses can occur.
Cathartic therapy can be viewed as an extinction procedure. Patients review traumatic memories while in a deeply relaxed state.
Ellis's REBT can be interpreted as a method for encouraging extinction of emotional reactions that previously caused problems. The client is encouraged to talk, but to do so calmly without "catastrophizing" or "awfulizing." If the therapy is successful, the stimuli lose their power to cause trouble.
Paradoxical therapy does the same thing by instructing a client to "make anxiety happen." This encourages a self-controlled, safe exposure to anxiety-causing thoughts.
For 30-40 years researchers documented the fact that two-thirds of people improved regardless of what they did about their psychological problems. Then researchers started to examine outcomes of specific therapies for specific problems.
For example, exposure therapies resulted in faster, more permanent "cures" for phobias than did talking therapies, reading therapies, and other approaches. However, exposure therapies were not suited to other problems, such as drug addiction.
After decades of therapy outcome research, a new phrase entered the lexicon of clinical psychologists: evidence-based therapy. The Google ngram viewer shows when that phrase emerged: around 1994.
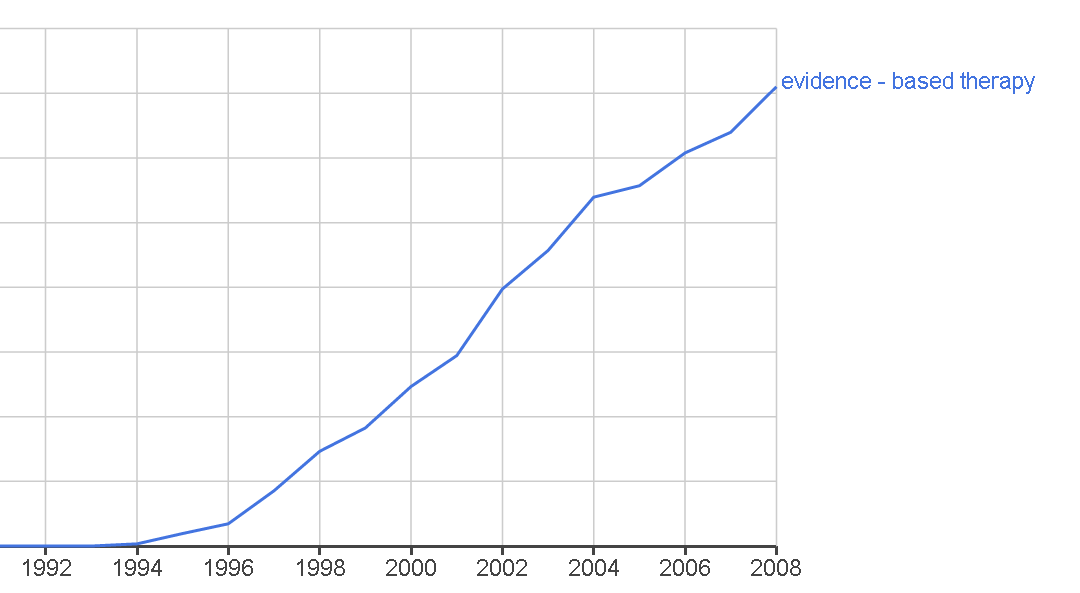
Google ngram data for "evidence-based therapy"
The data above only covers years up to 2008, which is what Google made publicly available in 2017, but the trend toward emphasizing evidence-based therapy continued to accelerate in the 21st Century. The idea comes from a general move toward evidence-
The ngram curve for evidence-based practice looks identical to the one for evidence-based therapy, above, so the two concepts co-evolved. Whether the underlying mechanism is extinction or not, psychologists are now mostly interested in therapies that make a demonstrable difference in helping people with their problems, in outcome research.
---------------------
References:
Cunningham, S (1984, February). Eysenck argues for conditioning theory of neurotic. APA Monitor, p.23.
Eysenck, H. (1952) The effects of psychotherapy: An evaluation. Journal of Consulting and Clinical Psychology, 16, 319-324.
Meldman, M. & Hatch, B. (1969) In vivo desensitization of an airplane phobia with penthranization. Behaviour Research and Therapy, 7, 213-214.
Jones, M.C. (1924) A laboratory study of fear: The case of Peter. Pedagogical Seminary, 31, 308-315. Retrieved from: https://psychclassics.yorku.ca/Jones/
Masserman, J.H. (1943) Behavior and Neurosis. Chicago: University of Chicago Press.
Wolpe, J. & Plaud, J.J. (1997) Pavlov's contributions to behavior therapy. American Psychologist, 52, 966-972.
Write to Dr. Dewey at psywww@gmail.com.
Don't see what you need? Psych Web has over 1,000 pages, so it may be elsewhere on the site. Do a site-specific Google search using the box below.
