Copyright © 2007-2018 Russ Dewey
Touch and Pain
The cutaneous sense or sense of touch involves three different types of receptors. One, the basket cell, consists of neural fibers wrapped around the base of a hair cell.
You can verify that a single basket cell, when stimulated, produces a detectable sensation. Find a single hair on your arm, carefully bend it without disturbing other hairs or pressing on your skin, and note the sensation. When the hair is bent by pressure, the neuron sends impulses to the brain.
What are basket cells? How can you stimulate one?
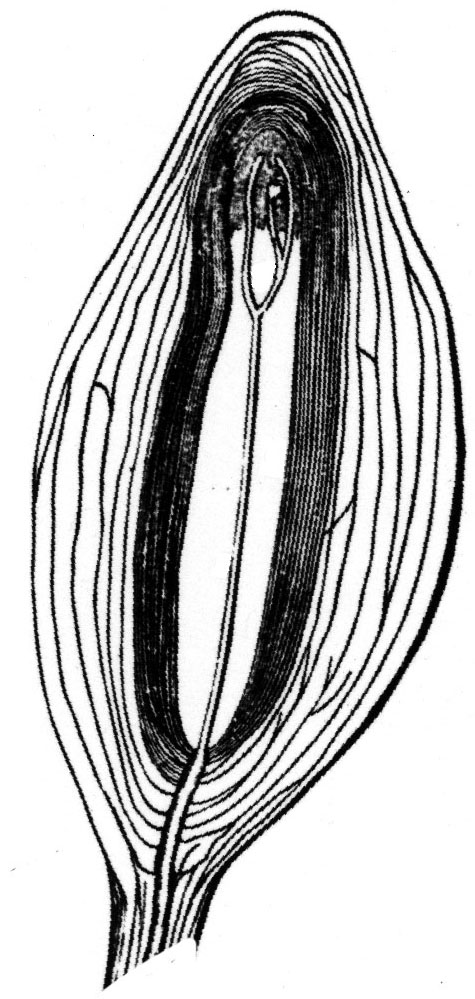
A single Pacinian corpuscle
On hairless skin such as fingertips, a receptor called the Pacinian corpuscle senses physical pressure to the skin. It consists of a multi-layered bag surrounding a sensitive nerve ending. Pressure to the bag triggers a nerve impulse.
A third type of touch receptor is the free nerve ending. It is simply a nerve fiber in the skin. Free nerve endings are sensitive to any sort of distortion, from pressure to tissue damage. Free nerve endings are the most numerous of the cutaneous receptors.
What is a Pacinian corpuscle?
Basket cells and Pacinian corpuscles are pressure receptors. Free nerve endings are pressure receptors and also temperature receptors. Pressure and temperature are the basic ingredients of the cutaneous sense.
What is a free nerve ending, and what can it sense that other touch receptors cannot?
Your sense of touch operates over time. Your brain is sensitive to overall patterns of cutaneous input that may be quite complex.
When you rub your fingertips (which are particularly rich in cutaneous receptors) over a surface like cloth, plastic, or wood, you feel a distinct texture. This is analogous to timbre in music.
Sensing texture involves thousands of touch receptors firing in sequence and in combination. This is called active touch and is used, for example, in reading Braille.
Braille is the system of writing for blind people invented by Louis Braille in 1824. Letters are represented by patterns of raised dots.
Expert readers of Braille report that they interpret the touch sensations automatically (without any conscious effort). This is just like expert readers of written words, who convert them into sounds without conscious effort.
How can the cutaneous sense become "educated"?
The motor cortex of the brain changes in response to experience with Braille reading. Areas devoted to touch sensations from fingertips grow larger.
Pain
The perception of pain is a complex topic. Clearly it depends upon special mechanisms in the brain, because some individuals are born without sensitivity to pain. This is called congenital indifference to pain or congenital analgesia.
The following case history from Magee (1963) illustrates the syndrome:
A 56-year-old white male insurance agent was first examined in 1957. He complained of muscle weakness that began at the age of 52...
During the patient's evaluation...it became apparent that he was indifferent to various types of painful stimuli on all parts of the body. The patient stated that this indifference had been present for as long as he could remember. There had been no tendency to develop greater appreciation of pain as he grew older.
He did not perceive itching and was not ticklish. As a child he could be lifted and pulled by the hair without crying or feeling upset. He could pull hair out of any part of his body without discomfort.
On several occasions, after injuring a fingernail, he had peeled off the whole nail without discomfort. He had noted, for example, that other people who struck their finger with a hammer would cry out with pain; however, he thought they were "sissies" and did not consider it abnormal when he did not react in the same manner.
He had received many burns and foreign particles had lodged in his eyes, but he had not felt pain... Despite his indifference to pain, the patient stated that he was quite aware of the intensity of painful or thermal stimuli.
Therefore, early in life he had learned, to a fairly satisfactory degree, to avoid situations that would harm him. Consequently, although he had received many injuries none was mutilating.
After injuries were incurred, they healed normally. The patient did complain of headache. He also noted that a full bladder produced an "uncomfortable" sensation, as did hunger...
...Testing of deep pain by squeezing the Achilles tendon or testicles produced no evidence of discomfort. Discrimination of degrees of temperature was also accurate; however, when sufficient heat was applied to burn the patient's skin, he made no movement to withdraw, nor did he show objective or subjective signs of pain.
...A skin and muscle biopsy were performed without anesthetic. The skin was removed without any sign of discomfort.
When the muscle was cut, the patient stated that he experienced a sensation that was "disagreeable," and therefore the surgeon injected local anesthetic. The patient did not think this necessary, stating that the disagreeable sensation was very mild. (p.47)
How did Magee's patient react to various kinds of pain?
Because congenital indifference to pain is inherited, there are whole families with the syndrome. It is not necessarily a blessing. Broken bones may go undetected and knit improperly; burns and rashes may go untreated.
In the case reported by Magee above, the man learned to detect stimuli caused by injuries, even though they were not painful. He lived to the age of 58, when he died of a heart attack. An autopsy disclosed abnormal tissue in a structure called the subcallosal fasciculus.
Scientists once assumed there were specific receptors for pain. Now it appears that pain sensations arise from free nerve endings: the same receptors that report normal touch sensations.
The brain does not receive pain signals directly. Pain perception requires a complex "gate" in the spinal cord to allow a combination of activities in cutaneous pathways.
Early brain scanning results suggested a distinctive response to pain of all kinds. Dubbed the "pain matrix," this pattern of activation appeared in hundreds of pain studies.
Then, as so often happens in science, additional research complicated the picture. A study by Salomons, Iannetti, Liang and Wood (2016) showed that patients with congenital indifference to pain had the same brain response in the so-called pain matrix of the brain, although they felt no pain. Researcher Tim Salomons concluded:
By testing people with no sense of pain, we can categorically rule out that these are pain-specific responses. ...These people still retain all other senses including non-painful touch, so the brain activity that has been dubbed the "pain matrix" is likely to represent these senses rather than actual pain.
Psychological influences on pain perception are well known. Several students reported experiences illustrating this.
Five months ago I became a certified paramedic with Metro ambulance in Atlanta. I then decided to come back to college. The head of the intramural football league found out I was a paramedic, and he hired me to work the football games. During my work with Metro and the football games, I have seen a lot of psychological reactions to pain.
I was called out on to Rotary Field a couple of weeks ago to help an injured person. When I arrived at the scene, there was a twenty-year-old boy lying on the ground.
He complained that his lower leg seemed strained. He did not show any reaction to pain other than slight discomfort.
I rolled up his sweats to his knee and found out what his discomfort was. The boy had a compound fracture of the tibia. The bone was partially out of his skin.
The boy wanted to see what was wrong but I told him not to look. He insisted on looking so I let him. Before I knew it he started screaming and fainted.
I brought him back around with an ammonia capsule. He did not look at his leg any more but was in great pain. [Author's files]
What are some anecdotes from students illustrate psychological factors in pain?
Another student had a dentist who was aware of psychological influences on pain:
Ever since my early childhood, the bi-annual trips to the dentist's office have caused me indescribable pain. Local anesthetics did not help. The deadening effects of Novocain had little effect on the pain caused by the drill.
It can be proven in my case that the pain comes not from my teeth but from somewhere else. I first noticed this when my new dentist, a bright young professional whom I will call Dr. L, illustrated my "ghost" pain to me by holding the drill in such a position that it was out of my sight.
My jaw was completely numb with Novocain. But as I heard the sound of the drill, a sharp pain shot the length of my body and I immediately became rigid and tense.
To my embarrassment, the only thing in my mouth was a metal probe. The drill was in Dr. L's opposite hand.
Dr. L then suggested that the pain was psychological. He didn't say that the pain was not real; on the contrary, he knew that psychological pain can be much worse that the slight discomfort experienced by most of his patients.
Using nitrous oxide, Dr. L was able to fill my cavities painlessly and easily. I will always be indebted to this doctor and thankful for his knowledge about pain. [Author's files]
Due to the role of the brain in pain perception, pain can often be relieved through psychological means. As discussed in Chapter 1, a placebo is a sugar pill or other treatment that works because people believe in it.
Placebo-induced pain relief apparently is due to the brain's ability to secrete natural pain-killing substances called endorphins. These substances resemble opiates such as morphine and heroin.
Why is placebo pain relief an example of mind/body interaction?
Although the effect is initiated or started through a psychological process (belief) the effect is physical and real. Jon Levine of the University of California found that placebo pain relief was equivalent to an 8 mg dose of morphine (Rensberger, 1987).
---------------------
References:
Geha, P. & Waxman, S. G. (2016) Pain perception: Multiple matrices or one? JAMA Neurology, 73, 628-630.
McGee, K. R. (1963) Congenital Indifference to Pain. Archives of Neurology, 9, 635-640. doi:10.1001/archneur.1963.00460120085009
Rensberger, B. (1987, January 10) Placebo's effect on pain may equal a dose of morphine. Washington Post. Retrieved from: https://www.washingtonpost.com/
Salomons, T. V., Iannetti, G., Liang, M., & Wood, J. (2016) The pain matrix in pain free individuals. JAMA Neurology, 73, 755-756. doi:10.1001/jamaneurol.
Write to Dr. Dewey at psywww@gmail.com.
Don't see what you need? Psych Web has over 1,000 pages, so it may be elsewhere on the site. Do a site-specific Google search using the box below.
